Scar prevention, management & improvement
Mr Olivier Amar - Leading Plastic Surgeon in Chelsea, London

Mr Olivier Amar is a leading expert in the treatment of scarring and is at the forefront of innovation. We are all prone to scars. Scars form naturally as part of the healing process after skin trauma. However, every person and every wound scars differently.
Scars can heal poorly if stitched quickly after an accident or emergency surgery, or because of trauma and damage to the tissue. Other reasons for poor scar healing may include leaving wounds untreated or exposing scars to the sun. Alternatively, you may scar excessively due to your genetics or skin type.
6 Types of scars
1. Keloids: Excessive collagen production, which continues even after wound healing, leads to tissue overgrowth above skin level. Keloid scars are initially purple or red and gradually fade over time. They are itchy and painful and may restrict movement when near a joint.
2. Contracture scars: Contracture scars are generally formed due to an injury that causes significant tissue loss, such as burns or injury to the joints. The skin and underlying tissue pull together for healing, often restricting movement.
3. Hypertrophic scars: Hypertrophic scars appear on the wound site in raised, thick, discolored clusters. Generally, they are uncomfortable and red, often widening with time.

4. Atrophic scars: Atrophic scars develop below the skin surface, producing a sunken appearance. They become more prominent with time due to aging.
5. Stretch marks: Striae, or stretch marks are formed due to breaks in the connective tissue, caused by rapid shrinking or growing of the skin. It is common with rapid weight loss, adolescence, pregnancy, and bodybuilding.
6. Acne scars: Scars are formed when a breakout penetrates the skin deeply and damages the tissues beneath it.
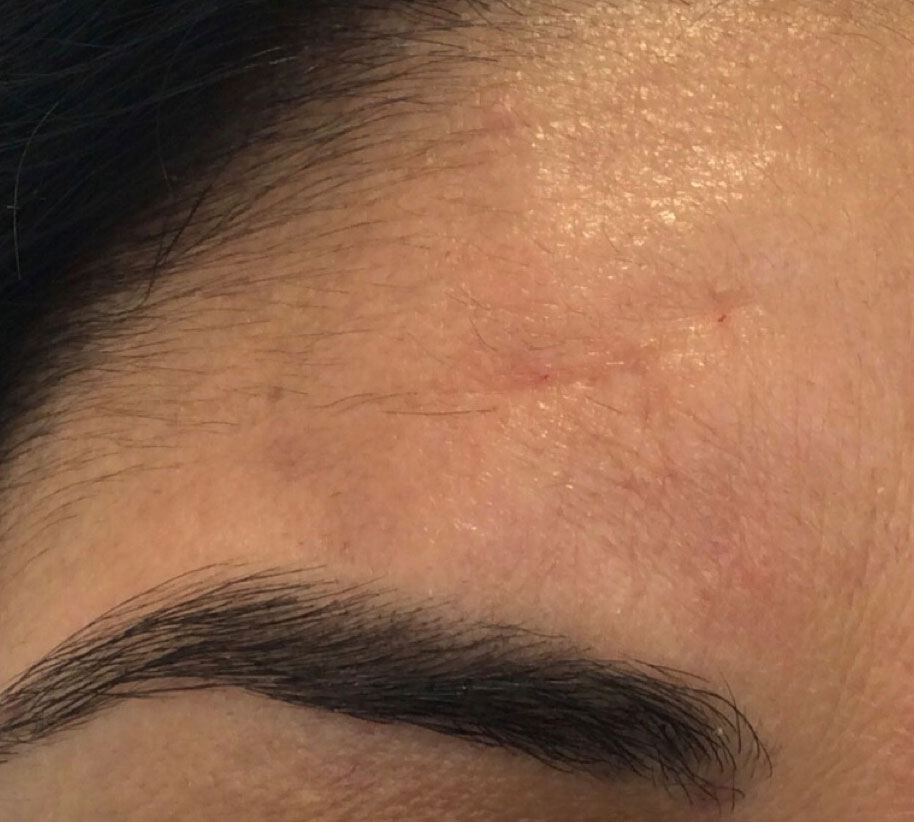
Mr Olivier Amar is highly experienced in scar management and offers many advanced treatments for existing scars. These include:
- Surgery to cut out excess scar tissue to leave a thinner, more unobtrusive scar.
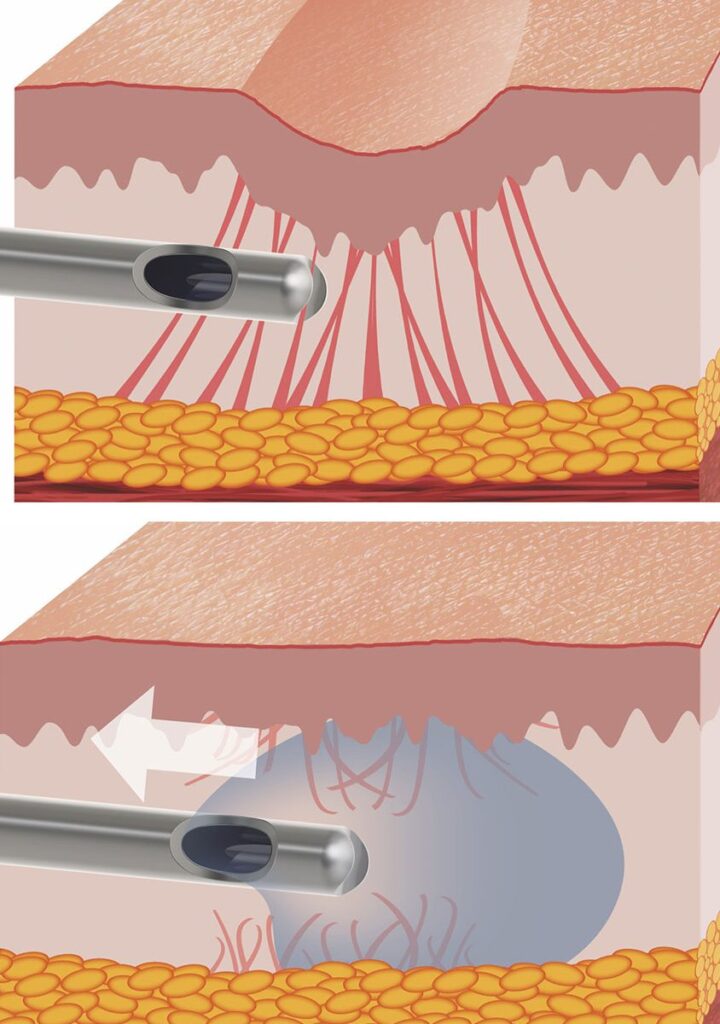
- Treatment of indented or depressed scars, such as acne scars. This type of scar is often ‘tethered’ to underlying tissues by tough fibres, in a similar way to a button on a mattress. Delicately cutting through these fibres permits the overlying skin to be released. Any remaining hollows can then be smoothed with fat transfer or dermal fillers as necessary (this treatment is called subcision).
- Laser treatment by Aerolase Neo to support healing, to help flatten scars and reduce redness and thickness.
- Specialist tattooing to restore natural-looking colour to pale scars.
- Fat transfer using nano fat to fill deep, hollow scars.
- Steroid injections to soften and reduce thick, red scars.
- Platelet Rich Plasma to improve healing and encourage normal collagen formation.
- Radiofrequency treatment by Renuvion to support skin tightening and healing.
Scars are very common but can cause a great deal of unhappiness. Scars may occur as a result of accidents, acne, burns, diseases or surgery. As a doctor and a researcher, I am dedicated to the management, prevention and improvement of scars.
Post-surgery, Mr Olivier Amar will monitor scar healing very carefully. A protocol may be initiated using steroid injections, silicone dressing and compression dressings to ensure the best possible result. This is particularly important if you have a history of scarring.
Did you know?
WHAT IS THE DIFFERENCE BETWEEN ‘GOOD’ AND ‘BAD’ SCARRING?
A ‘good’ scar fades significantly after appearing and blends in with the surrounding skin tone. A ‘poor’ scar, such as a keloid or hypertrophic scar, will stay visible and cause skin irritation for a number of months after formation. Time is the best healer as eventually normal scars and hypertrophic scars will mature and become pale.
WHAT CAN I DO TO ACHIEVE BETTER SCARS?
Scar quality will always vary from individual to individual and guarantees are impossible to give. There are ways to improve scars in the post-operative period for everyone with the use of various creams, oils and substances and thus we always advise our patients accordingly.
WHAT IS THE DIFFERENCE BETWEEN A HYPERTROPHIC SCAR AND A KELOID?
There is a whole range of scars but at the poor end there is the hypertrophic scar which occurs when the wound heals to become red, raised and itchy for a few months but will then resolve to become flat and pale. A keloid is similar but the scar continues to grow encroaching upon normal tissue and may need specific treatment.
WHAT ARE KELOIDS?
When a wound heals, it leaves a scar. A keloid is a special type of scar; one that grows too much and can even become larger than the original wound. It is not uncommon for surgical or injury scars to become a little lumpy (hypertrophic). A keloid differs from these in several ways:
- A keloid can come up after very minor skin damage, such as an acne spot, or even if there has been no obvious damage to the skin at all.
- It can spread outside the original area of skin damage.
- It may last permanently.
WHAT CAUSES KELOIDS TO OCCUR?
This is not fully understood. Most people never get keloids, others get them after the most minor of injuries. Several things affect the risk of getting one.
Dark skinned people get keloids much more easily than those with a paler skin. They are especially common in people with black skin. Keloids can crop up anywhere but do so most easily on certain areas, such as the skin around the upper chest and shoulders – particularly over the breastbone (sternum) – and on the earlobes. Having previously had a keloid increases the risk of getting another if subjected to trauma to their skin.
HOW CAN A SCAR AND KELOID BE TREATED?
Treatment is difficult and not always successful. Possible lines of treatments include the following:
- Injections of a steroid (triamcinolone) into a keloid may help to flatten small early ones.
- Steroid-impregnated tape applied for 12 to 24 hours a day may help to flatten keloids.
- Putting a silicone sheet over them at night for several months helps some keloids to flatten. Silicone in gel form is also available.
- Laser treatment makes scars and keloids less red, but does not make them smaller.
- If a scar or keloid is cut out, it usually comes back. This risk falls if the area is treated after the operation with pressure dressings or local steroid injections.





